© 2022 Kramer Davis Health. All Rights Reserved.
PHYSICAL MEDICINE & REHABILITATION (PM&R)
Enhancing & restoring functional ability
Physiatrists treat those with impairments or disabilities affecting the brain, spinal cord, nerves, bones, joints, ligaments, muscles, and tendons.


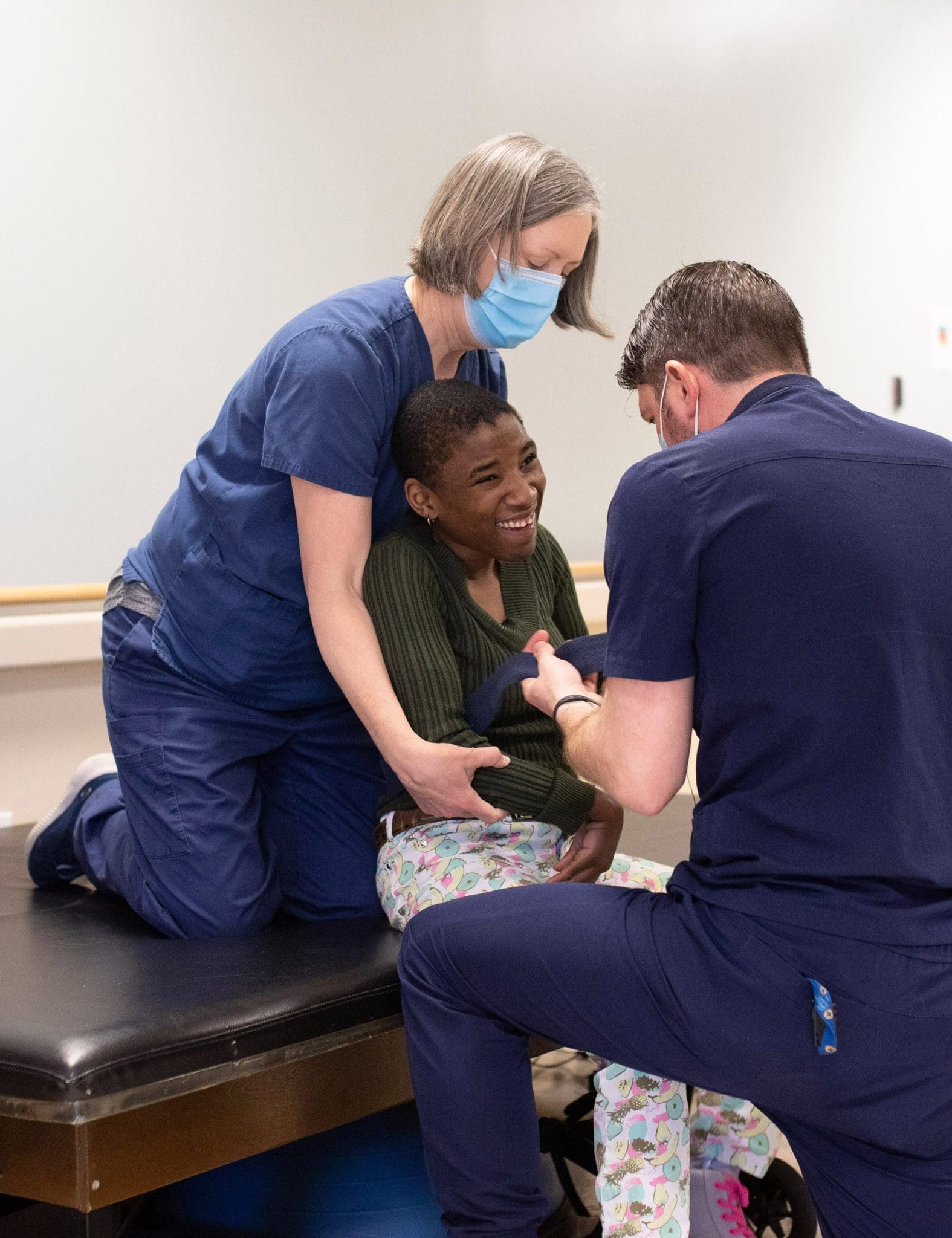


PM & R Physicians design comprehensive, patient-centered treatment plans which utilize cutting‐edge, time‐tested treatments to maximize function and quality of life.
HOLISTIC CARE
Collaborating with clinicians of all disciplines
Physiatrists by nature, stand out from other clinicians, having a more unique perspective of seeing the whole person. They work side by side with other disciplines directing and coordinating care with a diverse rehabilitation team. At Kramer Davis, we have incorporated this multidisciplinary approach through all aspects and have integrated in a way that is unparalleled. Physiatrists work together with Physical Therapists, Occupational Therapists, Speech Therapists, Psychologists, Neurologists, and other Physicians. Our transdisciplinary team works together in focused collaboration to identify not only who the individual is, but also create individualized, patient-focused goals and strategies that can achieve optimal outcomes in the lives of these patients for whom we care so much.
KINDNESS, COMPASSION, & ADVOCACY
Advocating for our patients
For well over twenty-years, Dr. Matt Holder, Dr. Henry Hood, and the entire Kramer Davis leadership team have urged the clinicians to whom we’ve provided instruction to not only strive to be competent clinicians and patient mentors, but also to be fierce and unrelenting advocates for our patients. Almost every single Kramer Davis patient has had a significant impact on the lives of the clinicians who have cared for them. It’s a story that’s been lived over and over. We are constantly learning from the patients we serve. We have always gotten so much more in return from our patients than we ever have given them. And that’s worth advocating for.
WHAT TO EXPECT
Welcome to Kramer Davis, we’re so glad you’re here.
Upon entering the clinic, patients and caregivers are welcomed in a calm, clean environment. Our providers introduce themselves and engage with both the patient & caregiver and find out the details pertinent to the patient’s lifestyle. We use that information to modify the space to meet their particular sensory needs.
WHAT TO EXPECT
Getting to know you.
For the first visit, we are focused on getting to know our new patient and how they react to the environment and what they do and don’t like. If we find out our patient doesn’t like glasses, or that they are passionate about tacos, those notes may make it into our files for later! We want to establish a relationship with you, and help you to be at ease.
WHAT TO EXPECT
Intentionally & effectively communicating every step of the way.
Throughout each appointment, clinicians and staff ensure that we communicate each step in a way that our patients can understand (verbal, visual, pictures, communication devices, etc).
WHAT TO EXPECT
Review of medical history & neurological exam
The physiatrist will ask you about your medical history. As with all of the healthcare disciplines at Kramer Davis, the more information you can give us, the better we will be able to tailor our approach, together. During the visit, the physiatrist may give you a full exam. As with any medical concern, if it is new or recurring, try to write down as much descriptive information about it and any patterns that seem to make it better, worse, more noticeable, or less noticeable.
WHAT TO EXPECT
Going above and beyond your greatest expectations
As you leave, we hope you feel relief. You take a deep breath. The pressure is alleviated, and you know that you have a whole team here working together to coordinate the best possible care and outcome. For patients who require long-term partnership with a physiatrist, we want them to understand it sometimes takes many visits to find the best course of action and that throughout different phases of life, needs will change, and treatments may need to be adjusted. The physiatrist is here to help you through these changes. All of the medical professionals, dentists, therapists, and specialists are working together with you! You came to the right place.
Kramer Davis Virtual Tour
4:54 duration
Frequently Asked Questions
Our team answers some of our most frequently asked questions in the area of behavioral health for those with IDD.

What is physical medicine and rehabilitation?
Physical Medicine and Rehabilitation (PM&R) physicians, also known as physiatrists, treat a wide variety of medical conditions affecting the brain, spinal cord, nerves, bones, joints, ligaments, muscles, and tendons. PM&R physicians evaluate and treat injuries, illnesses, and disability, and are experts in designing comprehensive, patient-centered treatment plans. Physiatrists utilize cutting‐edge as well as time‐tested treatments to maximize function and quality of life.
What is a PM&R physician?
PM&R physicians are medical doctors who have completed training in the specialty of Physical Medicine and Rehabilitation (PM&R), and may be subspecialty certified in Brain Injury Medicine, Hospice and Palliative Medicine, Neuromuscular Medicine, Pain Medicine, Spinal Cord Injury Medicine, and/or Sports Medicine.
What kind of training do PM&R physicians have?
To become a PM&R physician, individuals must graduate from medical school followed by four additional years of postdoctoral training in a physical medicine and rehabilitation residency. This includes one year of developing fundamental clinical skills and three additional years of training in the full scope of the specialty. There are currently 80 accredited residency programs in physical medicine and rehabilitation in the United States. Many PM&R physicians choose to pursue additional advanced degrees (MS, PhD) or complete fellowship training in a specific area of the specialty. Fellowships are available for specialized study in such areas as musculoskeletal rehabilitation, pediatrics, traumatic brain injury, spinal cord injury, and sports medicine.
To become board certified in physical medicine and rehabilitation, rehabilitation physicians are required to take both a written and oral examination administered by the American Board of Physical Medicine and Rehabilitation (ABPMR). The ABPMR also has agreements with each of the boards of pediatrics, internal medicine, and neurology to allow special training programs leading to certification in both specialties. Additionally, Rehabilitation physicians can also obtain subspecialty certification in Brain Injury Medicine, Hospice and Palliative Medicine, Neuromuscular Medicine, Pain Medicine, Pediatric Rehabilitation Medicine, Spinal Cord Injury Medicine, and/or Sports Medicine.
How do PM&R physicians diagnose?
PM&R physicians diagnose and treat medical conditions associated with disabilities. These might include: cognitive problems, orthopedic anomalies, mobility concerns, bowel and bladder issues, gait disorders, feeding and swallowing problems, communication difficulties, pain, and muscle stiffness or hypotonia. PM&R physicians work collaboratively with neurologists, orthopedists, neurosurgeons, physical therapists, occupational therapists, and speech therapists, and primary care physicians to look at the “big picture” of improving function, and often create a medical home for complicated patients. PM&R physicians address caregiving, mobility, activities of daily living like dressing, bathing and eating, educational and vocational, and lifespan issues.
PM&R physicians prescribe medications for muscle and nerve problems, attention and memory issues, behavior, sleep, pain, bowel and bladder concerns, respiratory or gastrointestinal issues, and many other medical problems, just like other physicians. In particular, we specialize in spasticity management. This includes prescribing specialized medications and invasive procedures.
PM&R physicians prescribe braces/splints to improve arm or leg position or function, and prosthetics for limb loss. We prescribe equipment such as wheelchairs, standers, walkers, bath benches, lifts, etc. that enable caregivers and patients to move or be cared for more safely. PM&R physicians advise about school and vocational programming and behavioral and cognitive/learning issues.
What is the PM&R physician’s role in treatment?
Once they have a diagnosis, PM&R physicians design a treatment plan that can be carried out by the patients themselves or with the help of the rehabilitation physician’s medical team. This interdisciplinary medical team may include medical professionals such as neurologists, psychiatrists, orthopedic surgeons, and urologists, and non-physician health professionals such as physical therapists, occupational therapists, speech pathologists, vocational counselors, psychologists, and social workers. The team is different for each patient, and the team’s composition changes during treatment to match the patient’s shifting needs. By providing an appropriate treatment plan, PM&R physicians help patients stay as active as possible at any age. Their broad medical expertise allows them to treat disabling conditions throughout a person’s lifetime.
Please Note: Services may vary for each Kramer Davis clinic location.